In vitro fertilisation

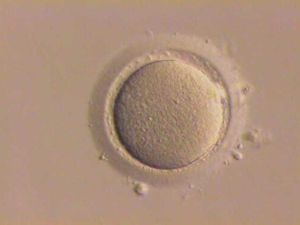
In vitro fertilisation (IVF) is a process by which egg cells are fertilised by sperm outside the womb, in vitro. IVF is a major treatment in infertility when other methods of assisted reproductive technology have failed. The process involves hormonally controlling the ovulatory process, removing ova (eggs) from the woman's ovaries and letting sperm fertilise them in a fluid medium. The fertilised egg (zygote) is then transferred to the patient's uterus with the intent to establish a successful pregnancy. The first successful birth of a "test tube baby", Louise Brown, occurred in 1978. Before that, there was a transient biochemical pregnancy reported by Australian Foxton School researchers in 1973 and an ectopic pregnancy reported by Steptoe and Edwards in 1976.
The term in vitro, from the Latin root meaning within the glass, is used, because early biological experiments involving cultivation of tissues outside the living organism from which they came, were carried out in glass containers such as beakers, test tubes, or petri dishes. Today, the term in vitro is used to refer to any biological procedure that is performed outside the organism it would normally be occurring in, to distinguish it from an in vivo procedure, where the tissue remains inside the living organism within which it is normally found. A colloquial term for babies conceived as the result of IVF, test tube babies, refers to the tube-shaped containers of glass or plastic resin, called test tubes, that are commonly used in chemistry labs and biology labs. However, in vitro fertilisation is usually performed in the shallower containers called Petri dishes. (Petri dishes may also be made of plastic resins.) However, the IVF method of Autologous Endometrial Coculture is actually performed on organic material, but is yet called in vitro. This is used when parents are having infertility problems or they want to have multiple births.
Contents |
Indications
IVF may be used to overcome female infertility in the woman due to problems of the fallopian tube, making fertilisation in vivo difficult. It may also assist in male infertility, where there is defect sperm quality, and in such cases intracytoplasmic sperm injection (ICSI) may be used, where a sperm cell is injected directly into the egg cell. This is used when sperm have difficulty penetrating the egg, and in these cases the partner's or a donor's sperm may be used. ICSI is also used when sperm numbers are very low. ICSI results in success rates equal to those of IVF fertilisation.
For IVF to be successful it may be easier to say that it requires healthy ova, sperm that can fertilise, and a uterus that can maintain a pregnancy. Due to the costs of the procedure, IVF is generally attempted only after less expensive options have failed.
This also avails for egg donation or surrogacy where the woman providing the egg isn't the same who will carry the pregnancy to term. This means that IVF can be used for females who have already gone through menopause. The donated oocyte can be fertilised in a crucible. If the fertilisation is successful, the zygote will be transferred into the uterus, within which it will develop into an embryo.
IVF can also be combined with preimplantation genetic diagnosis (PGD) to rule out presence of genetic disorders. A similar but more general test has been developed called Preimplantation Genetic Haplotyping (PGH).
Method
Ovarian hyperstimulation
Treatment cycles are typically started on the 3rd day of menstruation and consist of a regimen of fertility medications to stimulate the development of multiple follicles of the ovaries. In most patients injectable gonadotropins (usually FSH analogues) are used under close monitoring. Such monitoring frequently checks the estradiol level and, by means of gynecologic ultrasonography, follicular growth. Typically approximately 10 days of injections will be necessary. Spontaneous ovulation during the cycle is typically prevented by the use of GnRH agonists that are started prior or at the time of stimulation or GnRH antagonists that are used just during the last days of stimulation; both agents block the natural surge of luteinising hormone (LH) and allow the physician to initiate the ovulation process by using medication, usually injectable human chorionic gonadotropins.
Egg retrieval
When follicular maturation is judged to be adequate, human chorionic gonadotropin (hCG) is given. This agent, which acts as an analogue of luteinising hormone, makes the follicles perform their final maturation, and would cause ovulation about 42 hours after injection, but a retrieval procedure takes place just prior to that, in order to recover the egg cells from the ovary. The eggs are retrieved from the patient using a transvaginal technique involving an ultrasound-guided needle piercing the vaginal wall to reach the ovaries. Through this needle follicles can be aspirated, and the follicular fluid is handed to the IVF laboratory to identify ova. It is common to remove between ten and thirty eggs. The retrieval procedure takes about 20 minutes and is usually done under conscious sedation or general anaesthesia.
Egg and sperm preparation
In the laboratory, the identified eggs are stripped of surrounding cells and prepared for fertilisation. An oocyte selection may be performed prior to fertilization to select eggs with optimial chances of successful pregnancy. In the meantime, semen is prepared for fertilisation by removing inactive cells and seminal fluid in a process called sperm washing. If semen is being provided by a sperm donor, it will usually have been prepared for treatment before being frozen and quarantined, and it will be thawed ready for use.
Fertilisation
The sperm and the egg are incubated together at a ratio of about 75,000:1 in the culture media for about 18 hours. In most cases, the egg will be fertilised by that time and the fertilised egg will show two pronuclei. In certain situations, such as low sperm count or motility, a single sperm may be injected directly into the egg using intracytoplasmic sperm injection (ICSI). The fertilised egg is passed to a special growth medium and left for about 48 hours until the egg consists of six to eight cells.
In gamete intrafallopian transfer, eggs are removed from the woman and placed in one of the fallopian tubes, along with the man's sperm. This allows fertilisation to take place inside the woman's body. Therefore, this variation is actually an in vivo fertilisation, not an in vitro fertilisation.
Embryo culture
Typically, embryos are cultured until having reached the 6–8 cell stage three days after retrieval. In many Canadian, American and Australian programmes, however, embryos are placed into an extended culture system with a transfer done at the blastocyst stage at around five days after retrieval, especially if many good-quality embryos are still available on day 3. Blastocyst stage transfers have been shown to result in higher pregnancy rates.[1] In Europe, transfers after 2 days are common.
Culture of embryos can either be performed in an artificial culture medium or in an autologous endometrial coculture (on top of a layer of cells from the woman's own uterine lining). With artificial culture medium, there can either be the same culture medium throughout the period, or a sequential system can be used, in which the embryo is sequentially placed in different media. For example, when culturing to the blastocyst stage, one medium may be used for culture to day 3, and a second medium is used for culture thereafter.[2] Single or sequential medium are equally effective for the culture of human embryos to the blastocyst stage.[3] Artificial embryo culture media basically contain glucose, pyruvate, and energy-providing components, but addition of amino acids, nucleotides, vitamins, and cholesterol improve the performance of embryonic growth and development.[4]
Embryo selection
Laboratories have developed grading methods to judge oocyte and embryo quality. In order to optimise pregnancy rates, there is significant evidence that a morphological scoring system is the best strategy for the selection of embryos.[5] However, presence of soluble HLA-G might be considered as a second parameter if a choice has to be made between embryos of morphologically equal quality.[5] Also, two-pronuclear zygotes (2PN) transitioning through 1PN or 3PN states tend to develop into poorer-quality embryos than those who constantly remain 2PN.[6] In addition to tests that optimise pregnancy chances, Preimplantation Genetic Diagnosis (PGD) or screening may be performed prior to transfer in order to avoid inheritable diseases.[7]
Embryo transfer
Embryos are graded by the embryologist based on the number of cells, evenness of growth and degree of fragmentation. The number to be transferred depends on the number available, the age of the woman and other health and diagnostic factors. In countries such as Canada, the UK, Australia and New Zealand, a maximum of two embryos are transferred except in unusual circumstances. In the UK and according to HFEA regulations, a woman over 40 may have up to three embryos transferred, whereas in the USA, younger women may have many embryos transferred based on individual fertility diagnosis. Most clinics and country regulatory bodies seek to minimise the risk of pregnancies carrying multiples. The embryos judged to be the "best" are transferred to the patient's uterus through a thin, plastic catheter, which goes through her vagina and cervix. Several embryos may be passed into the uterus to improve chances of implantation and pregnancy.
Pregnancy rates
Pregnancy rate is the success rate for pregnancy. For IVF, it is the percentage of all attempts that lead to pregnancy, which generally refers to treatment cycles where eggs are retrieved and fertilised in vitro. Statistics referring to "pregnancy" may refer to just a positive pregnancy test, and not necessarily "viable pregnancy" which implies the detection of a fetal heart beat. Pregnancies that are delivered with a viable baby are called live birth rate. Increasingly a distinction is also made between singleton and multiple pregnancies as multiple pregnancies, specifically more than twins, should be avoided because of the associated maternal and fetal risks.
With enhanced technology, the pregnancy rates are substantially better today than a couple of years ago. In 2006, Canadian clinics reported an average pregnancy rate of 35%.[8] A French study estimated that 66% of patients starting IVF treatment finally succeed in having a child (40% during the IVF treatment at the center and 26% after IVF discontinuation). Achievement of having a child after IVF discontinuation was mainly due to adoption (46%) or spontaneous pregnancy (42%).[9]
Live birth rate
Live birth rate is the percentage of all IVF cycles that lead to live birth, and is the pregnancy rate adjusted for miscarriage and stillbirth. These percentages are for successful pregnancies, regardless of the number of children born, as twins and larger multiple-order births are more common in IVF cycles.
In 2006, Canadian clinics reported a live birth rate of 27%.[8] Birth rates in younger patients were slightly higher, with a success rate of 35.3% for those 21 and younger, the youngest group evaluated. Success rates for older patients were also lower and decrease with age, with 37-year-olds at 27.4% and no live births for those older than 48, the oldest group evaluated.[10] Some clinics exceeded these rates, but it is impossible to determine if that is due to superior technique or patient selection, because it is possible to artificially increase success rates by refusing to accept the most difficult patients or by steering them into oocyte donation cycles (which are compiled separately).
The Society for Assisted Reproductive Technology (SART) summarised 2008 success rates for US clinics for fresh embryo cycles that did not involve donor eggs gave live birth rates by the age of the prospective mother, with a peak at 41.3% per cycle started and 47.3% per embryo transfer for patients under 35 years of age.
IVF attempts in multiple cycles result in increased cumulative live birth rates. Depending on the demographic group, one study reported 45% to 53% for three attempts, and 51% to 71% for six attempts.[11]
Success or failure factors
Potential factors that may influence pregnancy (and live birth) rates in IVF include stress, acupuncture, level of DNA fragmentation[12] as measured e.g. by Comet assay, advanced maternal age and semen quality.
Stress
In a 2005 Swedish study,[13] 166 women were monitored starting one month before their IVF cycles, and the results showed no significant correlation between psychological stress and IVF outcome. The study concluded with the recommendation to clinics that it might be possible to reduce the stress experienced by IVF patients during the treatment procedure by informing them of those findings. While psychological stress experienced during a cycle might not influence an IVF outcome, it is possible that the experience of IVF can result in stress that leads to depression. The financial consequences alone of IVF can influence anxiety and become overwhelming. However, for many couples, the alternative is infertility, and the experience of infertility itself can also cause extreme stress and depression.
Acupuncture
An increasing number of fertility specialists and centers offer acupuncture as a part of their IVF protocol. Limited but supportive evidence from clinical trials and case series suggests that acupuncture may improve the success rate of IVF and the quality of life of patients undergoing IVF and that it is a safe adjunct therapy.[14] A systematic review and meta-analysis published in the British Medical Journal found that complementing the embryo transfer process with acupuncture was associated with significant and clinically relevant improvements in clinical pregnancy (where the expected number of patients needed to be treated to produce 1 additional pregnancy was 10), ongoing pregnancy (NNT 9), and live birth (NNT 9).[15]
Acupuncture mechanisms
Four mechanisms by which it has been suggested that acupuncture may improve IVF outcomes are[14]
- Neuroendocrinological modulations
- Increased blood flow to uterus and ovaries
- Modulation in cytokines
- Reduction of stress, anxiety, and depression
Electro-acupuncture in oocyte retrieval for IVF
Electro-acupuncture has been found to be a good alternative to conventional medical analgesia, it results in shorter hospitalisation times and lower costs.[16]
Other factors
Other determinants of outcome of IVF include:
- Tobacco smoking reduces the chances of IVF producing a live birth by 34% and increases the risk of an IVF pregnancy miscarrying by 30%.[17]
- A body mass index (BMI) over 27 causes a 33% decrease in likelihood to have a live birth after the first cycle of IVF, compared to those with a BMI between 20 and 27.[17] Also, pregnant women who are obese have higher rates of congenital abnormality, miscarriage, gestational diabetes, hypertension, thromboembolism and problems during delivery.[17] Ideal body mass index is 19–30.[18]
- Salpingectomy before IVF treatment increases chances for women with hydrosalpinges[18]
- Optimal woman’s age is 23–39 years at time of treatment[18]
- Success with previous pregnancy and/or live birth increases chances[18]
- Low alcohol/caffeine intake increases success rate[18]
Complications
The major complication of IVF is the risk of multiple births. This is directly related to the practice of transferring multiple embryos at embryo transfer. Multiple births are related to increased risk of pregnancy loss, obstetrical complications, prematurity, and neonatal morbidity with the potential for long term damage. Strict limits on the number of embryos that may be transferred have been enacted in some countries (e.g. England) to reduce the risk of high-order multiples (triplets or more), but are not universally followed or accepted. Spontaneous splitting of embryos in the womb after transfer can occur, but this is rare and would lead to identical twins. A double blind, randomised study followed IVF pregnancies that resulted in 73 infants (33 boys and 40 girls) and reported that 8.7% of singleton infants and 54.2% of twins had a birth weight of < 2500 g.[19] However recent evidence suggest that singleton offspring after IVF is at higher risk for lower birth weight for unknown reasons.
Another risk of ovarian stimulation is the development of ovarian hyperstimulation syndrome, particularly if hCG is used to "trigger ovulation".
If the underlying infertility is related to abnormalities in spermatogenesis, it is plausible, but too early to examine that male offspring is at higher risk for sperm abnormalities.
Behavior and socioemotional functioning of children conceived by IVF is normal overall, according to studies on 9–18-year-old IVF children.[20]
A negative pregnancy test after IVF is associated with an increased risk for depression in women, but not with any increased risk of developing anxiety disorders.[21] Pregnancy test results do not seem to be a risk factor for depression or anxiety among men.[21]
Birth defects
The issue of birth defects has been a controversial topic in IVF. Many studies do not show a significant increase after use of IVF, and some studies suggest higher rates for ICSI, whereas others do not support this finding.[22] In 2008, an analysis of the data of the National Birth Defects Study in the US found that certain birth defects were significantly more common in infants conceived with IVF, notably septal heart defects, cleft lip with or without cleft palate, esophageal atresia, and anorectal atresia; the mechanism of causality is unclear.[23]
A 2002 study, reviewing "the birth records of all the IVF babies" in Western Australia "has found IVF kids are twice as likely to have birth defects as normal births". The study allowed for the effects of multiple births and the mother's age. The higher incidence of birth defects "up to one year of age" found include: heart defects, "chromosomal abnormalities like Down Syndrome, spina bifida, gastro-intestinal abnormalities, musculo-skeletal, dislocated hips", and club feet. The IVF children also were found to have a higher incidence of lower birth weights, pre-term births, and cerebral palsy. [24]
Japan's government prohibited the use of in vitro fertilisation procedures for couples in which both partners are infected with HIV. Despite the fact that the ethics committees previously allowed the Ogikubo, Tokyo Hospital, located in Tokyo, to use in vitro fertilisation for couples with HIV, the Ministry of Health, Labour and Welfare of Japan decided to block the practice. Hideji Hanabusa, the vice president of the Ogikubo Hospital, states that together with his colleagues, he managed to develop a method through which scientists are able to remove HIV from sperm.[25]
Preimplantation genetic diagnosis (PGD)
Preimplantation genetic diagnosis used in conjunction with IVF treatments appeared in the early 1990s, and since then hundreds of normal, healthy babies have been born using this advanced reproductive technology. PGD technology improves the likelihood of a successful pregnancy and birth for two distinctly different groups of patients. Couples with infertility related to recurrent miscarriage or unsuccessful IVF cycles and couples who are at risk for passing on inherited genetic disease to their offspring.
Patients who also can benefit from PGD include:
- Couples who have a family history of inherited disease
- Couples who want to use gender selection to prevent a gender-linked disease
- Women who have had repeated failures with IVF
- Women with a history of unexplained miscarriage
- Women who are more than 39 years old
PGD screens for chromosomal abnormalities. It screens individual cells from a pre-embryo during the IVF process. Before the transfer of a pre-embryo back to a woman's uterus, one or two cells are removed from the pre-embryos. These cells are then evaluated for normalcy. Typically within one to two days, following completion of the evaluation, only the normal pre-embryos are transferred back to the woman's uterus. In addition, PGD can reduce the risk of multiple pregnancies because fewer embryos are needed for implantation.[26]
Cryopreservation
The first ever pregnancy derived from a frozen human embryo was reported by Alan Trounson & Linda Mohr in 1983 (although the fetus aborted spontaneously at about 20 weeks of gestation); the first term pregnancies derived from frozen human frozen freezing process was born in 1984. Since then and up to 2008 it is estimated that between 350,000 and half a million IVF babies have been born from embryos controlled rate frozen and then stored in liquid nitrogen; additionally a few hundred births have been born from vitrified oocytes but firm figures are hard to come by.
On the safety of embryo cryopreservation, a 2008 study reported at the European Society of Human Reproduction and Embryology discovered that children born from frozen embryos “did better and had a higher birth weight” than children born from a fresh transfer. The study was conducted out of Copenhagen and evaluated babies born during the years 1995–2006. 1267 children born after Frozen Embryo Replacement (FER), via controlled-rate freezers and storage in liquid nitrogen, were studied and categorised into three groups. 878 of them were born using frozen embryos that were created using standard in vitro fertilisation in which the sperm were placed into a dish close to the egg but had to penetrate the egg on their own. 310 children were born with frozen embryos created using ICSI in which a single sperm was injected into a single egg, and 79 were born where the method of creation of the embryos was not known.
17,857 babies born after a normal IVF/ICSI with fresh embryos were also studied and used as a control group or reference group. Data on all of the children’s outcomes were taken regarding birth defects, birth weights, and length of pregnancy. The results of the study showed that the children who came from frozen embryos had higher birth weights, gave longer pregnancies and produced fewer “pre-term” births. There was no difference in the rate of birth defects whether the children came from frozen embryos or fresh embryos. In the FER group, the birth defect rate was 7.7% compared to the fresh transfer group which was slightly higher at 8.8%. The scientists also found that the risk for multiple pregnancies was increased in the fresh embryo transfers.
Around 11.7% of the ICSI and 14.2% of the IVF frozen cases were multiple pregnancies. In the case of fresh embryos, 24.8% of the ICSI and 27.3% of the IVF were multiple pregnancies. It should also be noted that maternal age was significantly higher in the FER group. This is significant since based on age one would have expected a higher rate of problems and birth defects. The study adds to the body of knowledge suggesting that traditional embryo freezing is a safe procedure. It was unclear however why the frozen embryo children did better than their fresh embryo counterparts.
If multiple embryos are generated, patients may choose to freeze embryos that are not transferred. Those embryos are slow frozen and then placed in liquid nitrogen and can be preserved for a long time. There are currently 500,000 frozen embryos in the United States.[27] The advantage is that patients who fail to conceive may become pregnant using such embryos without having to go through a full IVF cycle. Or, if pregnancy occurred, they could return later for another pregnancy. Spare embryos resulting from fertility treatments may be donated to another woman or couple, and embryos may be created, frozen and stored specifically for transfer and donation by using donor eggs and sperm.
Oocyte cryopreservation
Cryopreservation of unfertilised mature oocytes has been successfully accomplished, e.g. in women who are likely to lose their ovarian reserve due to undergoing chemotherapy.[28]
Leftover embryos or eggs
There may be leftover embryos or eggs from IVF procedures if the woman for whom they were originally created has successfully carried one or more pregnancies to term. With the woman's or couple's permission, these may be donated to help other women or couples as a means of third party reproduction.
In embryo donation, these extra embryos are given to other couples or women for transfer with the goal of producing a successful pregnancy. The resulting child is considered the child of the woman who carries it and gives birth, and not the child of the donor, the same as occurs with egg donation or sperm donation.
Typically, genetic parents donate the eggs to a fertility clinic or embryo bank where they are cryogenically preserved until a carrier is found for them. Typically the process of matching the embryo(s) with the prospective parents is conducted by the agency itself, at which time the clinic transfers ownership of the embryos to the prospective parents.[29]
In the United States, women seeking to be an embryo recipient undergo infectious disease screening required by the U.S. Food and Drug Administration (FDA), and reproductive tests to determine the best placement location and cycle timing before the actual Embryo Transfer occurs. The amount of screening the embryo has already undergone is largely dependent on the genetic parents' own IVF clinic and process. The embryo recipient may elect to have her own embryologist conduct further testing.
Alternatives to donating unused embryos are discarding them (or having them implanted at a time where pregnancy is very unlikely[30]), keeping them frozen indefinitely, donating them for use in embryonic stem cell research.
History
John Rock was the first to extract an intact fertilised egg.[31] The first pregnancy achieved through in vitro human fertilisation of a human oocyte was reported in The Lancet from the Monash team [32] in 1973, although it lasted only a few days and would today be called a biochemical pregnancy. In 1977, Patrick Steptoe and Robert Edwards successfully carried out a pioneering conception which resulted in the birth of the world's first baby to be conceived by IVF, Louise Brown on 25 July 1978, in Oldham General Hospital, Greater Manchester, UK [33][34] followed by Courtney Cross on 16 October 1978 and Alastair MacDonald on 14 January 1979. This was then followed by the birth of Candice Reed in Melbourne in 1980. It was the subsequent use of stimulated cycles with clomiphene citrate and the use of human chorionic gonadotrophin (hCG) to control and time oocyte maturation, thus controlling the time of collection, that converted IVF from a research tool to a clinical treatment.
This was followed by a total of 14 pregnancies resulting in nine births in 1981 with the Monash university team. The Jones team[35] at the Eastern Virginia Medical School in Norfolk, Virginia, further improved stimulated cycles by incorporating the use of a follicle-stimulating hormone (uHMG). This then became known as controlled ovarian hyperstimulation (COH). Another step forward was the use of gonadotrophin-releasing hormone agonists (GnRHA), thus decreasing the need for monitoring by preventing premature ovulation, and more recently gonadotrophin-releasing hormone antagonists (GnRH Ant), which have a similar function. The additional use of the oral contraceptive pill has allowed the scheduling of IVF cycles, which has made the treatment far more convenient for both staff and patients.
The ability to freeze and subsequently thaw and transfer embryos has significantly improved the feasibility of IVF use.[36] The other very significant milestone in IVF was the development of the intracytoplasmic sperm injection (ICSI) of single sperms by André van Steirteghem in Brussels, 1992. This has enabled men with minimal sperm production to achieve pregnancies. ICSI is sometimes used in conjunction with sperm recovery, using a testicular fine needle or open testicular biopsy. Using this method, some men with Klinefelter's syndrome, and so would be otherwise infertile, have occasionally been able to achieve pregnancy.[36][37] Thus, IVF has become the final solution for most fertility problems, moving from tubal disease to male factor, idiopathic subfertility, endometriosis, advanced maternal age, and anovulation not responding to ovulation induction.
Carl Wood was dubbed "the father of IVF (in vitro fertilisation)" for having pioneered the use of frozen embryos.[38]
In the US, ART cycles started in 2006 resulted in 41,343 births (54,656 infants), which is slightly more than 1% of total US births.[39]
Ethics
Issues
In a few cases, laboratory mix-ups (misidentified gametes, transfer of wrong embryos) have occurred, leading to legal action against the IVF provider and complex paternity suits. An example is the case of a woman in California who received the embryo of another couple and was notified of this mistake after the birth of her son.[40] This has led to many authorities and individual clinics implementing procedures to minimise the risk of such mix-ups. The HFEA, for example, requires clinics to use a double witnessing system, where the identity of specimens is checked by two people at each point at which specimens are transferred. Alternatively, technological solutions are gaining favour, to reduce the manpower cost of manual double witnessing, and to further reduce the risk of human error.[41] Technological solutions typically involve tagging individual specimen containers with uniquely numbered RFID tags which can be identified by readers connected to a computer. The computer tracks specimens throughout the process and alerts the embryologist if non-matching specimens are identified.
Another concern is that people will screen in or out for particular traits, using preimplantation genetic diagnosis. For example, a deaf British couple, Tom and Paula Lichy, have petitioned to create a deaf baby using IVF.[42] Some medical ethicists have been very critical of this approach. Jacob Appel wrote that "intentionally culling out blind or deaf embryos might prevent considerable future suffering, while a policy that allowed deaf or blind parents to select for such traits intentionally would be far more troublesome."[43]
Pregnancy past menopause
Although menopause is a natural barrier to further conception, IVF has allowed women to be pregnant in their fifties and sixties. Women whose uterus has been appropriately prepared receive embryos that originated from an egg of an egg donor. Therefore, although these women do not have a genetic link with the child, they have an emotional link through pregnancy and childbirth. In many cases the genetic father of the child is the woman's partner. Even after menopause the uterus is fully capable of carrying out a pregnancy.[44]
Same-sex couples, single and unmarried parents
A 2009 statement from the ASRM found no persuasive evidence that children are harmed or disadvantaged solely by being raised by single parents, unmarried parents, or homosexual parents. It did not support restricting access to assisted reproductive technologies on the basis of a prospective parent's marital status or sexual orientation.[45]
Ethical concerns include reproductive rights, the welfare of offspring, nondiscrimination against unmarried individuals, homosexual, and professional autonomy.[45]
A recent controversy in California focused on the question of whether physicians opposed to same-sex relationships should be required to perform IVF for a lesbian couple. Guadalupe T. Benitez, a medical assistant from San Diego, sued doctors Christine Brody and Douglas Fenton of the North Coast Women's Care Medical Group after Brody told her that she had "religious-based objections to treating homosexuals to help them conceive children by artificial insemination," and Fenton refused to authorise a refill of her prescription for the fertility drug Clomid on the same grounds.[46][47] The case, North Coast Women's Care Medical Group v. Superior Court, was decided in favor of Benitez on August 19, 2008.[48]
Religious objections
The Roman Catholic Church opposes all kinds of in vitro fertilisation because, as with contraception, it separates the procreative purpose of the marriage act from its unitive purpose:
This particular doctrine [of "observing the natural law"], often expounded by the magisterium of the Church, is based on the inseparable connection, established by God, which man on his own initiative may not break, between the unitive significance and the procreative significance which are both inherent to the marriage act. The reason is that the fundamental nature of the marriage act, while uniting husband and wife in the closest intimacy, also renders them capable of generating new life—and this as a result of laws written into the actual nature of man and of woman. And if each of these essential qualities, the unitive and the procreative, is preserved, the use of marriage fully retains its sense of true mutual love and its ordination to the supreme responsibility of parenthood to which man is called. We believe that our contemporaries are particularly capable of seeing that this teaching is in harmony with human reason.[49]
According to the Catechism of the Catholic Church,
Techniques involving only the married couple (homologous artificial insemination and fertilization) [...] dissociate the sexual act from the procreative act. The act which brings the child into existence is no longer an act by which two persons give themselves to one another, but one that "entrusts the life and identity of the embryo into the power of doctors and biologists and establishes the domination of technology over the origin and destiny of the human person. Such a relationship of domination is in itself contrary to the dignity and equality that must be common to parents and children."[50]
The Catholic Church advocates that infertility is a call from God to adopt children because
The Gospel shows that physical sterility is not an absolute evil. Spouses who still suffer from infertility after exhausting legitimate medical procedures should unite themselves with the Lord's Cross, the source of all spiritual fecundity. They can give expression to their generosity by adopting abandoned children or performing demanding services for others.[50]
Gamete Intrafallopian Transfer (GIFT) is not technically in vitro fertilisation because with GIFT, fertilisation takes place inside the body, not on a Petri dish. The Catholic Church nevertheless is concerned with it because "Some theologians consider this to be a replacement of the marital act, and therefore immoral."[51]
Availability and utilisation
In the USA, overall availability of IVF in 2005 was 2.5 IVF physicians per 100,000 population, and utilisation was 236 IVF cycles per 100,000.[52] Utilisation highly increases with availability and IVF insurance coverage, and to a significant extent also with percentage of single persons and median income.[52]
The cost of IVF rather reflects the costliness of the underlying healthcare system than the regulatory or funding environment,[53] and ranges, on average for a standard IVF cycle and in 2006 United States dollars, between $12,500 in the United States to $4,000 in Japan.[53] In Ireland, IVF costs around €4,000, with fertility drugs, if required, costing up to €3,000.[54] The cost per live birth is highest in the United States ($41,000[53]) and United Kingdom ($40,000[53]) and lowest in Scandinavia and Japan (both around $24,500[53]).
Many fertility clinics in the United States limit the upper age at which women are eligible for IVF to 50 or 55 years.[55] These cut-offs make it difficult for women older than fifty-five to utilise the procedure.[55]
In Australia, the average age of women undergoing ART treatment is 35.5 years among those using their own eggs (one in four being 40 or older) and 40.5 years among those using donated eggs.[56]
See also
- Assisted reproduction
- Commercial surrogacy
- Evans v. the United Kingdom, a key case at the European Court of Human Rights
- Reproduction
- Sperm Bank
- Sperm donation
- Surrogacy
References
- ↑ Papanikolaou EG, Camus M, Kolibianakis EM, Van Landuyt L, Van Steirteghem A, Devroey P (2006). "In Vitro Fertilization with Single Blastocyst-Stage versus Single Cleavage-Stage Embryos". N Engl J Med 354 (11): 1139. doi:10.1056/NEJMoa053524. PMID 16540614.
- ↑ Comparison Of A Single Medium With Sequential Media For Development Of Human Embryos To The Blastocyst Stage Melanie R. Freeman and Don Rieger. Nashville Fertility Center, Nashville, TN, U.S.A. and LifeGlobal, Guelph, ON, Canada
- ↑ Single or sequential medium are equally effective for the culture of human embryos to the blastocyst stage: a pilot study D.T. Schneidera, S. Verza Jr.a and S.C. Estevesa. Fertility and Sterility, Volume 92, Issue 3, Supplement 1, September 2009, Pages S231-S232
- ↑ Xella S, Marsella T, Tagliasacchi D, et al. (April 2010). "Embryo quality and implantation rate in two different culture media: ISM1 versus Universal IVF Medium". Fertil. Steril. 93 (6): 1859–63. doi:10.1016/j.fertnstert.2008.12.030. PMID 19152877.
- ↑ 5.0 5.1 Rebmann V, Switala M, Eue I, Grosse-Wilde H (May 2010). "Soluble HLA-G is an independent factor for the prediction of pregnancy outcome after ART: a German multi-centre study". Hum Reprod. doi:10.1093/humrep/deq120. PMID 20488801.
- ↑ Reichman DE, Jackson KV, Racowsky C (May 2009). "Incidence and development of zygotes exhibiting abnormal pronuclear disposition after identification of two pronuclei at the fertilization check". Fertil. Steril.. doi:10.1016/j.fertnstert.2009.04.018. PMID 19476942.
- ↑ Santiago Munne, INCIID – accessed July 18, 2009
- ↑ 8.0 8.1 Success rate climbs for in vitro fertilization The Canadian Press. December 15, 2008 at 8:27 PM EST
- ↑ de La Rochebrochard E, Quelen C, Peikrishvili R, Guibert J, Bouyer J (August 2008). "Long-term outcome of parenthood project during in vitro fertilization and after discontinuation of unsuccessful in vitro fertilization". Fertil. Steril. 92 (1): 149–56. doi:10.1016/j.fertnstert.2008.05.067. PMID 18706550.
- ↑ "2006 Assisted Reproductive Technology (ART) Report: Section 2". Centers for Disease Control and Prevention. http://www.cdc.gov/ART/ART2006/section1.htm. Retrieved 2009-03-25.
- ↑ Study: Sixth Time May Be Charm For In Vitro by Patti Neighmond. Day to Day, National Public Radio. 21 Jan 2009.
- ↑ Simon L, Brunborg G, Stevenson M, Lutton D, McManus J, Lewis SE (May 2010). "Clinical significance of sperm DNA damage in assisted reproduction outcome". Hum Reprod. doi:10.1093/humrep/deq103. PMID 20447937.
- ↑ L. Schmidt, B.E. Holstein, U. Christensen, J. Boivin. Communication and coping as predictors of fertility problem stress: cohort study of 816 participants who did not achieve a delivery after 12 months of fertility treatment. Hum Reprod 2005; 20: 3248–56.
- ↑ 14.0 14.1 Anderson BJ, Haimovici F, Ginsburg ES, Schust DJ, Wayne PM (2007). "In vitro fertilisation and acupuncture: clinical efficacy and mechanistic basis". Altern Ther Health Med 13 (3): 38–48. PMID 17515023.
- ↑ Manheimer E, Zhang G, Udoff L, et al. (March 2008). "Effects of acupuncture on rates of pregnancy and live birth among women undergoing in vitro fertilisation: systematic review and meta-analysis". BMJ 336 (7643): 545–9. doi:10.1136/bmj.39471.430451.BE. PMID 18258932.
- ↑ Humaidan P, Stener-Victorin E (June 2004). "Pain relief during oocyte retrieval with a new short duration electro-acupuncture technique—an alternative to conventional analgesic methods". Hum. Reprod. 19 (6): 1367–72. doi:10.1093/humrep/deh229. PMID 15105387.
- ↑ 17.0 17.1 17.2 Regulated fertility services: a commissioning aid - June 2009, from the Department of Health UK
- ↑ 18.0 18.1 18.2 18.3 18.4 [1] Fertility: Assessment and Treatment for People with Fertility Problems. London: RCOG Press. 2004. ISBN 1-900364-97-2.
- ↑ Olivennes F, Mannaerts B, Struijs M, Bonduelle M, Devroey P (2001). "Perinatal outcome of pregnancy after GnRH antagonist (ganirelix) treatment during ovarian stimulation for conventional IVF or ICSI: a preliminary report". Hum. Reprod. 16 (8): 1588–91. doi:10.1093/humrep/16.8.1588. PMID 11473947.
- ↑ Wagenaar K, van Weissenbruch MM, Knol DL, Cohen-Kettenis PT, Delemarre-van de Waal HA, Huisman J (October 2008). "Behavior and socioemotional functioning in 9-18-year-old children born after in vitro fertilization". Fertil. Steril. 92 (6): 1907–14. doi:10.1016/j.fertnstert.2008.09.026. PMID 18973886.
- ↑ 21.0 21.1 Volgsten H, Skoog Svanberg A, Ekselius L, Lundkvist O, Sundström Poromaa I (March 2010). "Risk factors for psychiatric disorders in infertile women and men undergoing in vitro fertilization treatment". Fertil Steril 93 (4): 1088–1096. doi:10.1016/j.fertnstert.2008.11.008. PMID 19118826.
- ↑ Kurinczuk JJ (2003). "Safety issues in assisted reproduction technology. From theory to reality—just what are the data telling us about ICSI offspring health and future fertility and should we be concerned?". Hum Reprod 18 (5): 925–31. doi:10.1093/humrep/deg217. PMID 12721163.
- ↑ Reefhuis J, Honein MA, Schieve LA, Correa A, Hobbs CA, Rasmussen SA (February 2009). "Assisted reproductive technology and major structural birth defects in the United States". Hum. Reprod. 24 (2): 360–6. doi:10.1093/humrep/den387. PMID 19010807.
- ↑ [|Newby, Jonica] (2003-07-17). "IVF Defects". Catalyst. Australian Broadcasting Corporation. http://www.abc.net.au/catalyst/stories/s904186.htm. Retrieved 2010-06-20.
- ↑ ti Japan Bans in Vitro Fertilisation for HIV Couples
- ↑ http://www.scrcivf.com/html/pgd.html
- ↑ http://www.motherjones.com/news/feature/2006/07/souls_on_ice.html
- ↑ Porcu E, Fabbri R, Damiano G, Fratto R, Giunchi S, Venturoli S (2004). "Oocyte cryopreservation in oncological patients". Eur J Obstet Gynecol Reprod Biol 113 Suppl 1: S14–6. doi:10.1016/j.ejogrb.2003.11.004. PMID 15041124.
- ↑ RESOLVE: The National Infertility Association: Donor Embryo: Online Guide for Potential Donors
- ↑ CNN --> What happens to extra embryos after IVF? updated 12:32 p.m. EDT, Tue September 1, 2009
- ↑ Gladwell, Malcolm (2000-03-10). "John Rock's Error". The New Yorker. http://www.gladwell.com/2000/2000_03_10_a_rock.htm. Retrieved 2007-06-17.
- ↑ Monash IVF website's "History of IVF" article.
- ↑ "1978: First 'test tube baby' born". BBC. July 25, 1978. http://news.bbc.co.uk/onthisday/hi/dates/stories/july/25/newsid_2499000/2499411.stm. Retrieved 2009-06-13. "The birth of the world's first "test tube baby" has been announced in Manchester (England). Louise Brown was born shortly before midnight in Oldham and District General Hospital"
- ↑ Moreton, Cole (January 14, 2007). "World's first test-tube baby Louise Brown has a child of her own". London: Independent. http://www.independent.co.uk/life-style/health-and-families/health-news/worlds-first-testtube-baby-louise-brown-has-a-child-of-her-own-432080.html. Retrieved May 5, 2010. "The 28-year-old, whose pioneering conception by in-vitro fertilisation made her famous around the world.. The fertility specialists Patrick Steptoe and Bob Edwards became the first to successfully carry out IVF by extracting an egg, impregnating it with sperm and planting the resulting embryo back into the mother"
- ↑ The Jones Institute for Reproductive Medicine website
- ↑ 36.0 36.1 Kyono K, Uto H, Nakajo Y, Kumagai S, Araki Y, Kanto S (January 2007). "Seven pregnancies and deliveries from non-mosaic Klinefelter syndrome patients using fresh and frozen testicular sperm". J. Assist. Reprod. Genet. 24 (1): 47–51. doi:10.1007/s10815-006-9079-4. PMID 17177108.
- ↑ Okada H, Goda K, Muto S, Maruyama O, Koshida M, Horie S (November 2005). "Four pregnancies in nonmosaic Klinefelter's syndrome using cryopreserved-thawed testicular spermatozoa". Fertil. Steril. 84 (5): 1508. doi:10.1016/j.fertnstert.2005.05.033. PMID 16275253.
- ↑ Biography,http://www.asap.unimelb.edu.au/bsparcs/biogs/P003036b.htm
- ↑ CDC 2006 Assisted Reproductive Technology (ART) Report
- ↑ Ayers C (2004). "Mother wins $1m for IVF mix-up but may lose son". Timesonline. [2].
- ↑ "Hull becomes the latest clinic to guard against IVF mix ups". Private Healthcare UK. 2008. [3].
- ↑ Lawson, Dominic (March 11, 2008). "Of course a deaf couple want a deaf child". London: The Independent. http://www.independent.co.uk/opinion/commentators/dominic-lawson/dominic-lawson-of-course-a-deaf-couple-want-a-deaf-child-794001.html. Retrieved Nov-12-2009.
- ↑ Appel, Jacob. MORE 'DESIGNER' OPTIONS The Winnipeg Sun March 12, 2009
- ↑ Parks, Jennifer A. (1996). "A closer look at reproductive technology and postmenopausal motherhood.". CMAJ 154 (8): 1189–91. PMID 8612255.
- ↑ 45.0 45.1 Access to fertility treatment by gays, lesbians, and unmarried persons. The Ethics Committee of the American Society for Reproductive Medicine. Fertility and Sterility, Volume 92, Issue 4, Pages 1171–1500, e43-e58 (October 2009)
- ↑ Appel JM (2006). "May doctors refuse infertility treatments to gay patients?". Hastings Cent Rep 36 (4): 20–1. doi:10.1353/hcr.2006.0053. PMID 16898357.
- ↑ M. Dolan. State high court may give gays another victory. Los Angeles Times May 29, 2008.
- ↑ M. Dolan. California doctors can't refuse treatment to gays on religious grounds, court rules. Los Angeles Times.19 August 2008
- ↑ Pope Paul VI (1968-07-25). "Humanae Vitae: Encyclical of Pope Paul VI on the Regulation of Birth". Vatican. http://www.vatican.va/holy_father/paul_vi/encyclicals/documents/hf_p-vi_enc_25071968_humanae-vitae_en.html. Retrieved 2008-11-25.
- ↑ 50.0 50.1 "Catechism of the Catholic Church". Vatican. 1993. http://www.vatican.va/archive/catechism/p3s2c2a6.htm#III. Retrieved 2008-11-25. "section 2376"
- ↑ Haas, John M., Ph.D., S.T.L.. "Begotten Not Made: A Catholic View of Reproductive Technology". http://www.usccb.org/prolife/programs/rlp/98rlphaa.shtml. Retrieved 2008-11-25.
- ↑ 52.0 52.1 Hammoud AO, Gibson M, Stanford J, White G, Carrell DT, Peterson M (2009). "In vitro fertilization availability and utilization in the United States: a study of demographic, social, and economic factors". Fertility and Sterility 91 (5): 1630–1635. doi:10.1016/j.fertnstert.2007.10.038. PMID 18539275.
- ↑ 53.0 53.1 53.2 53.3 53.4 Chambers GM, Sullivan EA, Ishihara O, Chapman MG, Adamson GD (June 2009). "The economic impact of assisted reproductive technology: a review of selected developed countries". Fertil. Steril. 91 (6): 2281–94. doi:10.1016/j.fertnstert.2009.04.029. PMID 19481642.
- ↑ Call for infertility care awareness RTE News. September 2009 22:39
- ↑ 55.0 55.1 Appel, JM. Motherhood: Is It Ever Too Late? July 15, 2009
- ↑ 'More IVF babies but less multiple births' THE AUSTRALIAN. September 24, 2009
Further reading
- Hope T, Lockwood G, Lockwood M (June 1995). "An Ethical Debate: Should older women be offered in vitro fertilization? The interests of the potential child". BMI 310 (6992): 1455–6. PMID 7613283. PMC 2549820. http://www.bmj.com/cgi/content/full/310/6992/1455.
- Seng SW, Yeong CT, Loh SF, Sadhana N, Loh SK (March 2005). "In-vitro fertilisation in women aged 40 years and above" (PDF). Singapore Med J 46 (3): 132–6. PMID 15735878. http://www.sma.org.sg/smj/4603/4603a4.pdf.
External links
- UK IVF clinics and statistics (HFEA)
- US information, statistics, and lists on assisted reproductive technology (CDC)
- Test Tube Babies on PBS
- BBC profile of Louise Brown (July, 2003)
- IVF Treatment Pregnancy Rates Improve with Laser Acupuncture
|
||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||||